How do I exercise with diabetes while staying in range
Exercising with diabetes and keeping blood sugar balanced is possible and over time I can testify that it even becomes easy provided you do it right. What it means? In this article, I will list key principles with which I manage to exercise and stay balanced. I came to these insights after quite a bit of blood, sweat and tears – literally. After years of running long distances, participating in competitions and quite a few years as a bodybuilder, when part of the time I was based on a high-carbohydrate diet and for a short period even on a vegan diet. You can say that I made quite a few mistakes along the way. Those who follow me know that for years I have been basing my meals on animal foods “from head to tail” and that I limit the amount of carbohydrates I eat. This is how I manage to balance the blood sugar to the values of a person who does not have diabetes (70-100 mg/dl). My goal is not to avoid carbohydrates completely but to limit them to a level where I will not see an increase in blood sugar levels after eating them.
This article is important for all diabetics who wish to engage in sports and at the same time maintain balanced blood sugar, whether it is an amateur or professional sports activity, type 1 or type 2 diabetics, young and old, men and women. I believe that the principles that I will list in the article will be able to shorten the way for you to a quality and balanced workout and prevent in advance unnecessary drops and jumps in sugar, some of which may be life-threatening. Beyond that, maintaining physical fitness and physical strength will help prevent diabetes complications in the future and improve the quality of life in the present. In some cases of type 2 diabetes, if we catch the disease at a relatively early stage, organized and intense training can be, among other things, the answer to the complex question – how to prevent diabetes.
So how do we manage to train and maintain a high level of performance when we eat a minimal amount of carbohydrates? All this while maintaining a balanced blood sugar?
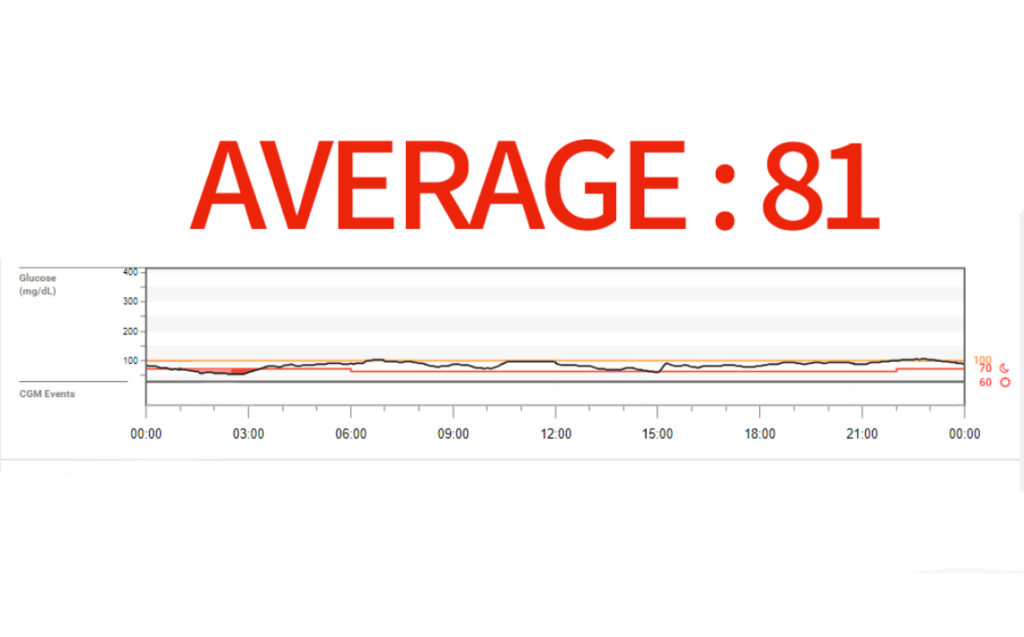
Table of contents:
Fitness and diabetes – aerobic and anaerobic with diabetes
Before we talk about exercise and diabetes, I want to define the two main ways to exercise. Muscles are made up of long fibers that shorten and contract when they perform work such as lifting weights or moving the body. All muscle fibers require high-energy molecules derived from glucose or fatty acids in order to function. One part of the muscle fibers are the fibers that utilize aerobic metabolism to produce high energy from small amounts of glucose and oxygen. These fibers can withstand light loads for prolonged periods of time and are the most effective for “aerobic” activity, such as running, long distance walking, dancing, easy swimming, cycling at medium speed and other activities that are not particularly intense.
The second part of the muscle fibers are the fibers designed for lifting heavy loads for a short time. They require energy at a rapid rate, so they must be able to produce a tremendous amount of energy in a shorter time than the rate at which the heart is able to pump blood to supply available oxygen. This metabolic process is called anaerobic metabolism and is carried out, among other things, with the help of those muscle fibers that require larger amounts of glucose to perform intense and fast activity.
Blood sugar levels during prolonged exercise
Physical activity has quite an effect on blood sugar levels, and for this reason it will probably make it difficult to balance blood sugar, especially for those taking blood sugar lowering medications such as insulin or metformin. As you know, insulin is not exactly a drug but a hormone.
Prolonged physical exertion will lower blood sugar levels due to the efficiency of glucose transfer in the muscle cells. In most cases the drop in blood sugar levels will be sudden. The blood sugar will drop suddenly under the following conditions: the effort must be prolonged, insulin must be present in the blood in sufficient quantity and the blood sugar cannot be too high.
Blood sugar levels during strength training
There is a myth in the medical world that says that physical activity lowers blood sugar levels. It’s not entirely accurate. Strenuous and fast training such as intense weight training, high intensity swimming, sprints and tennis will cause an immediate release of stress hormones such as epinephrine and cortisol and they in turn signal the liver and muscles to release glucose into the bloodstream by converting glycogen from the glycogen stores into glucose. In a non-diabetic person, in response to an increase in blood sugar levels, the pancreas will release small amounts of insulin, thus preventing high concentrations of blood sugar. For a type 2 diabetic patient in the intermediate stage, when the pancreas is still releasing small amounts of insulin, the blood sugar level will rise for a certain period of time but eventually – will fall back down thanks to the delayed insulin response. As mentioned, short and strenuous physical activity may increase blood sugar levels, while prolonged physical activity will almost always lead to a decrease in blood sugar levels. Type 1 diabetics whose pancreas no longer produces insulin will need a bolus of insulin during intense and fast training. You should consult your doctor about this.
Balance with fast carbohydrates
The bodies of people who do not take drugs to lower blood sugar levels are able to react in time and “cancel” the drop in sugar that occurs after the secretion of insulin from the pancreas during prolonged exercise, but it will be impossible to “turn off” an injection of insulin or a large amount of metformin after taking them. To avoid a dangerous situation of extremely low blood sugar, physical activity must be “covered” with glucose tablets in advance, before the drop in blood sugar levels. Most of the tablets sold in Israel and around the world come in a box of about 10 tablets, with each tablet containing 4 grams of glucose. Read the exact sugar concentration on the box before use. It is not recommended to use fruits or other sweet treats because the result will not be as accurate as when using glucose tablets and the effect of fruits or treats will often be too slow to be used during physical activity. The slow breakdown of some of the carbohydrates found in certain fruits or desserts can cause an excessively high level of blood sugar hours after eating them, thus making efforts to balance blood sugar more difficult. Therefore, glucose tablets made of dextrose are the most suitable for physical activity thanks to their speed of action and accuracy.
Correct dosage and timing of carbohydrates
Trial and error is required to know how many carbohydrates we should take to cover the training in the best way. At a time when we are adjusting the dose of carbohydrates during training, the blood sugar meter will be the best tool for accurate monitoring and monitoring of the changes in blood sugar. When a person with an average weight of 64 kg eats a glucose tablet containing 4 grams of glucose, his blood sugar level will increase by about 10 mg/dL. Since the glucose tablets raise blood sugar levels in less than 5 minutes, they are ideal for use during relatively short physical activity. Before training, the first thing you need to do is check your blood sugar level and remember the result or even write it down on a journal page so that you know how to change dosages in the following trainings if necessary. If your blood sugar is below range, take enough tablets to bring it back up to target. Wait about half an hour for the tablet to finish working and if you haven’t reached your goal yet, you may be too weak to train effectively. The first few times you train, my advice is to take half a tablet at the beginning of the workout and half a tablet every 15 minutes after that. In the beginning period when you are still learning how your body reacts to training, check your blood sugar level even in the middle of the training to make sure it does not drop to too low values. Always make sure you leave with enough tablets to cover the workout and if the blood sugar is indeed low, it should be brought back up and continue the workout. If it is too high you may have to stop training and I know how frustrating it can be for people who love sports – but at least during the adjustment period it may be necessary. It is always important to remember that true fitness is built over years. Giving up one workout is meaningless compared to building real fitness that lasts for years.
after training
Measure the blood sugar level again and if necessary fix it with tablets. During the learning period, it is important to remember and even write down all blood sugar values and the exact time of
Every measurement and every tablet. About an hour after the end of the workout, check the blood sugar level again. If the sugar continues to drop in the hour after the end of the workout, then this too must be corrected with tablets. Intense or prolonged physical activity can cause drops in blood sugar for hours and even for a day after the end of the workout and it will usually be necessary to make adjustments to the insulin doses during these hours.
After you have collected the data, it is time to calculate – if you used a total of 6 tablets, it can be assumed that in the next workout you will have to take 6 tablets divided into equal amounts, one every 15 minutes during the workout. It is important to remember that different types of training will affect blood sugar differently.
Repeat the data collection once every few months and especially while you make changes to your training program. If you added another type of training such as strength training to your aerobic program, or if you decided to increase the intensity of the training – it may be necessary to add additional glucose tablets to cover the training or alternatively to prepare with an insulin injection for intense strength training at certain times of the day, especially in the morning. More details on training times below.
Physical fitness, insulin sensitivity and diabetes
Insulin sensitivity usually improves dramatically with weight loss and as the ratio of abdominal fat to lean body mass decreases. Prolonged or strenuous physical activity reduces insulin resistance at that moment regardless of changes in muscle mass. Insulin sensitivity varies equally whether the insulin is produced by the body or whether the insulin is injected externally. As sensitivity improves insulin becomes more effective in lowering blood sugar levels and if you inject insulin you will likely need to reduce doses when you start a new exercise program.
The build-up of fat naturally caused by the action of insulin will also decrease, so we will probably expect a decrease in muscle mass during this period. In my experience, daily physical activity over time will cause an increase in insulin sensitivity. Over time the high sensitivity will stabilize at a certain sensitivity level. This prolonged stability remains in the body for about two weeks when we stop exercising and it is important to be aware of this especially for those who inject insulin. About two weeks after stopping the training program, the insulin doses will probably need to be increased according to the gradual increase in blood sugar levels. If for some reason you do not have the opportunity to exercise for a week, most likely the increased sensitivity to insulin will remain as it is. Building muscle mass also increases the sensitivity to insulin at rest, but in this situation it will often take many months of bodybuilding before you notice changes in blood sugar levels while resting. Muscles by themselves improve insulin sensitivity.
Building muscle mass with a low-carb diet
These are questions I hear a lot – how can you develop a mass with diabetes and a low-carbohydrate diet? Is it possible to combine a ketogenic diet and sports? This can be done by increasing the amount of protein we consume and if there really is no choice, to increase muscle mass relatively quickly, we can also gradually increase the amount of carbohydrates we consume to increase the body’s demand for insulin. By increasing the amount of carbohydrates and increasing the amount of insulin required, we will encourage the building of muscle mass. Muscle mass is built with resistance training such as weight lifting. If you train correctly, i.e. gradually and with enough trees – lifting weights is better than aerobic training. Aerobic activity is physical activity that is moderate enough to provide oxygen to the muscles during the activity. When we train aerobically, we hardly develop muscle mass, partly because the muscles will hardly require glucose for energy. Anaerobic physical activity that deprives the muscles of oxygen exhausts the muscles relatively quickly and requires 20 times the amount of glucose required to perform the same amount of work by aerobic activity. When performing anaerobic activity, the muscles break down the following day, but at the end of the day, the muscles begin a building process that will last on average another day. Hence the recommendation to carry out high-intensity weight training in a one-day-no-day format. Such an interval gives the body 48 hours of rest between workouts. Muscle mass increases insulin sensitivity regardless of physical activity. Muscles require a large amount of available energy in order to function. When muscle mass increases, the efficiency of glucose transfer also increases and the efficiency of insulin use in the cell increases in accordance with the increase in muscle mass.

When should diabetics avoid exercise
First of all, when the blood sugar level is high – 160 mg/dL or higher. This number varies from person to person, but overall a high level of blood sugar will cause the sugar to rise during exercise. This effect will be less dramatic for type 2 diabetics whose pancreas is still producing insulin but it will be dramatic for type 1 diabetics who have not covered the rise in blood sugar with insulin.
It is not recommended to exercise shortly after an insulin injection, and it is even advisable to wait at least 3 hours after the last bolus injection, unless it is a strenuous workout that raises blood sugar levels.
Most type 1 diabetics will need to inject an additional rapid insulin bolus when they exercise in the morning, but not when they exercise in the afternoon. This is a good example of the effect of the stress hormones that are secreted in the hours after waking up and cause increases in blood sugar for no apparent reason. Dr. Richard K. Bernstein called this phenomenon the “dawn syndrome” and type 1 diabetics will testify that when they exercise in the afternoon, blood sugar levels almost always drop during exercise.
Restrictions on physical activity with diabetes
It is important to remember that as a diabetic you should consult your doctor before you decide to take part in a strenuous exercise program. Before any change towards a sporty lifestyle, parameters such as: age, heart condition, blood sugar balance, weight, the number of years you have had diabetes and whether you have diabetes complications must be taken into account. The doctor knew how to take these parameters into account and determine what type of physical activity you can perform and at what intensity.
In conclusion
After the learning period the benefits you will experience from adding regular training to your daily routine will outweigh the disadvantages. One major advantage is the prevention of future diabetes complications, beyond the immediate benefits such as improving physical sensation and mood.
The main disadvantage of physical activity for insulin-dependent diabetics is the difficulty in controlling blood sugar levels, during and after physical exertion. If you apply the principles detailed in this article, there is no reason why you won’t be able to exercise and maintain a balanced blood sugar, provided you don’t make too fast and extreme changes, that is, you implement each change gradually. Gradualness is the key word that accompanies every insulin-dependent diabetic throughout his life. You will find that over time, exercising with diabetes becomes easier and more predictable and that there is no obstacle to exercising at a high intensity with diabetes and a low-carb diet. The myth that “you can’t build muscle mass without carbohydrates” is not true and has been disproved quite a few times by famous athletes and bodybuilders like Dr. Sיhawn Baker.
The secret is to consume sufficient amounts of animal food, with an emphasis on sufficient amounts of protein and never to be too hungry or force ourselves to fast. Sometimes, as a start, it is necessary to eat larger amounts than the amounts you are used to, but over time this too should balance out. Spot coverage of certain workouts with carbohydrates and spot coverage of certain workouts with insulin are necessary to maintain a straight line of blood sugar before, during and after exercise. I believe that for diabetics who limit the amount of carbohydrates and base their meals on quality animal food, the sky is the limit and therefore there should be no obstacle to participating in almost all types of competitive sports that exist, provided that balancing diabetes is a priority. After adapting to this way of eating and as long as you eat good amounts of protein and fat and you don’t starve your body, you will see that your physical fitness will be better than the days when you ate carbohydrates and that the recovery time from training to training is getting shorter even when it comes to training trees.
The story of Tomer who went through my “Manage Diabetes” program:
Tomer – Type 1 diabetes came to me unbalanced when he was determined to balance to the levels of a person without diabetes so that he could return to his love: professional sports and in Tomer’s case – bodybuilding and weightlifting. His ultimate goal was to eventually reach the national championship as a regular competitor. Tomer ended up participating in the competition and much more than that, he competed while relying solely on a clean and real diet. ‘On the road’ he deals with this complex and everyday phenomenon called type 1 diabetes. It is not obvious and Tomer has proven that it is possible to engage in such a demanding sport without and to remain balanced, without supplementing the body with all kinds of substances or stimulants of all kinds. This is Tomer’s real victory.
I think Tomer summed up the process more accurately than I did: “Because I was not satisfied with the results, I started being accompanied by a nutritionist diagnosed with juvenile diabetes like myself, Tomer Pepe. Tomer taught me a lot of things, he taught me to balance my sugar in the most accurate way possible, he taught me that in order to be balanced and become a competitive athlete I need to create a routine for myself as regular as possible, like a professional athlete does, in order to balance my sugar levels and progress further Faster. When I came to Tomer my a1c was 7.2, today it is 4.8.
From my giving up the pastas, pizzas and ice creams, I gained a body that I am happy with, I gained to lift weights that I never imagined I could lift, I took something out of my life to fill it with something else.” – Tomer Gerdinger.

*The information on this website is not intended to be a substitute for professional medical advice, diagnosis or treatment. The said information is intended for informational purposes only and stems from personal experience. The text is not intended to diagnose, treat or cure any specific disease or medical condition. Reviews and testimonials about nutrition, training and various health approaches represent individual experiences and what is stated on the site does not guarantee any results for your specific situation. Any choice of a specific way of eating or medical treatment according to a given situation should be made under the guidance of professionals qualified to do so.