What insulin has to do with hunger?
I guess you know the feeling that comes after finishing a meal rich in carbohydrates. We finished eating lunch and half an hour later we are hungry again and we feel weak and shaky. The next step will usually be a quick walk to the fridge or the pantry trying to get an energy boost from a snack, it could be a piece of chocolate, a cookie or even some nuts, only to feel hungry again shortly after and so on. Others will make themselves some caffeinated drink on that occasion. The craving for coffee often results from a disruption in daily energy balance. A healthy and metabolically flexible person will probably not suddenly have cravings for coffee. When we are not metabolically healthy, such situations which represents some sort of energy deficiency may arise in our cells and thus in our body. The sudden desire for a cup of coffee only to get a short boost of energy often stems from the brain signaling us that the body is in an energy crisis.
I believe that everyone can relate to this kind of situation at some point in life. In this article, I will explain the relationship between insulin and feelings of hunger. This is a relationship which I know personally as a type 1 diabetic who checks blood sugar levels daily. I will try to add to my explanations the background of those other hormones that affect feelings of hunger and satiety, besides insulin.
insulin
Insulin is a peptide hormone produced by beta cells in the pancreatic islets and is considered one of the most important anabolic hormones in the body. Insulin allows the cells to absorb glucose for energy, or to store it in the form of fat in the liver and muscles.
In people who do not live with diabetes, insulin is secreted continuously. The body should ideally produce the necessary amount of insulin according to its needs and the food that is consumed. For example, after a meal, blood sugar levels rise and the pancreas secretes extra insulin, which keeps blood sugar levels, within normal limits.
Therefore, insulin help cells absorb sugar correctly. Insulin has many other functions, but its main function is to balance in blood and in cell sugar levels.
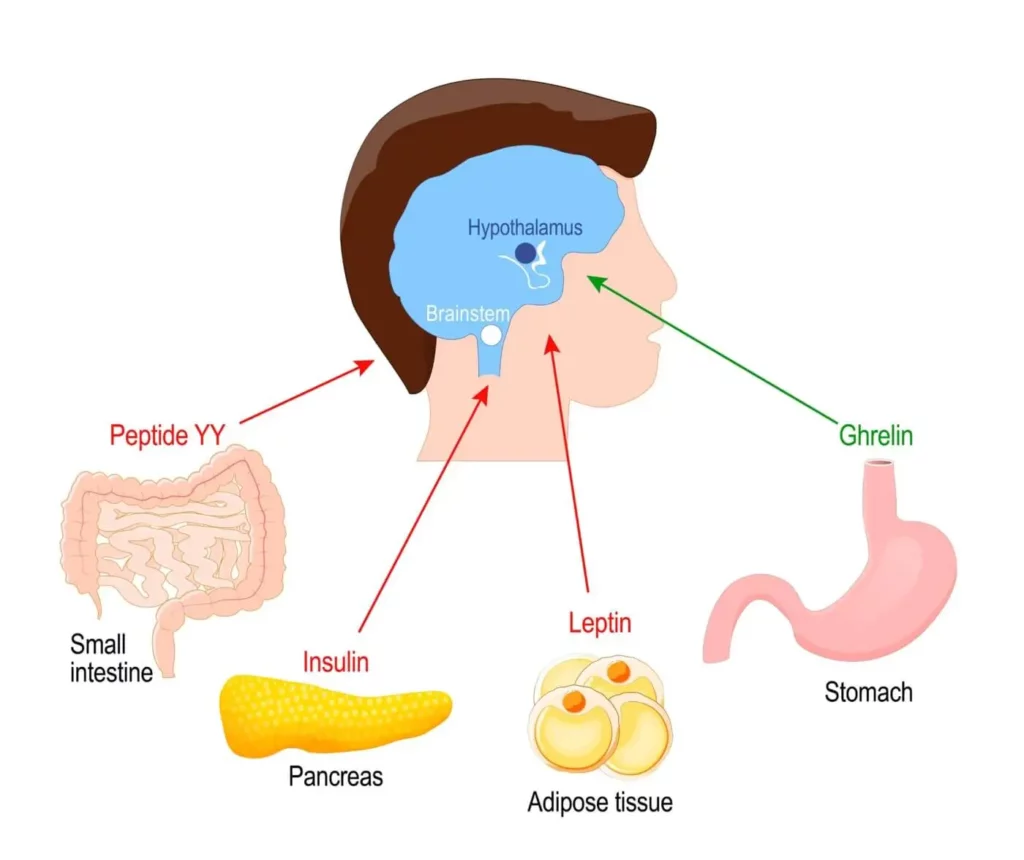
Leptin and Ghrelin
Two hormones that are known to play an important role in balancing energy levels in the body. The role of leptin “the satiety hormone” is to regulate the energy balance by suppressing food intake and thus it also indirectly encourages weight loss. Ghrelin, the “hunger hormone”, has the opposite action of leptin and its activity time is faster. With the release of ghrelin, the body send us signals that it is time to absorb new sources of energy into the body.
Insulin levels rises as a response to the rise in blood sugar levels at the end of a high-carbohydrate meal. After the insulin has finished regulating blood sugar levels, leptin levels will rise to send us signals that we have enough energy and there is no need for additional food consumption. The action of leptin will cause slower absorption of insulin and by that leptin will gradually reduce insulin production. Thus, leptin and ghrelin rise and fall throughout the day according to the activity of insulin and according to changes in blood sugar levels.
Relationship between insulin and hunger mechanism to the metabolic syndrome
All body systems affect each other and depend on each other. When insulin rises and falls throughout the day as a result of eating large amounts of carbohydrates, a vicious cycle is created that disrupts the natural secretion of hormones in the axis: leptin-ghrelin-insulin-thyroid hormones-stress hormones. When insulin rises and falls over time, instability will occur which may cause resistance to some of these hormones. One resistance that has become relatively “famous” called- insulin resistance. Prolonged resistance to insulin and insulin that rises and falls throughout the day may eventually cause an erosion of the production and regulation of insulin amounts by the pancreas, and an increase in the amount of insulin in the blood. High insulin in the blood over time leads to problems such as: obesity, metabolic syndrome or type 2 diabetes and most of modern world diseases known for us today.
In my opinion, there is only one way to get out of this vicious cycle and that is a to follow a diet that wisely restrict carbohydrates intake to the amount that will be unseen in blood glucose levels. Each person can find the right amount which will depend on medical conditions, metabolic status, age, and other factors. An in depth health care professional should be consulted here in order to assess the level of carbohydrate tolerance and the efficiency of insulin response.
On a personal note
I know from my experience that when my blood sugar drops even a little below 80 mg\dl for example to a level around 70 mg\dl, I can feel a sudden pang of hunger. Could it be that these small changes are the ones that control the hunger-satiety mechanism in our body? Could this be the only reason us humans feel hungry in nature?
The balance of hunger and satiety in the body is flatten when we switch to a diet in which we limit the amount of carbohydrates from food, provided that we do it correctly by offering the body full spectrum of nutrients it requires in order to function optimally, without starving ourselves, without forcing ourselves to fast and without forcing ourselves to eat.
One of the least understood mechanisms in the body in my opinion is the mechanism stands behind the feeling of hunger and satiety.
After I measure my blood sugar level and the glucometer shows a value of 70 mg/dl, I correct with one glucose tablet and at the same moment that blood sugar climbs back to 85 mg/dl, hunger disappears. Obvious question is:
Is real hunger in nature exists?
Or could it be that every feeling of hunger in our bodies and in the whole mammal family is a direct result of some sort of a mild hypoglycemia?
It is possible that we will never feel hungry if we do not eat for a few days and with the help of a correct dose of external or internal insulin, we will be able to keep blood sugar levels at around 85 mg/dL without fluctuations?
These are questions that come to my mind from time to time. There is a need for qualitative studies that will investigate these questions more in depth.
*The information on this website is not intended to be a substitute for professional medical advice, diagnosis or treatment. The said information is intended for informational purposes only and stems from personal experience. The text is not intended to diagnose, treat or cure any specific disease or medical condition. Reviews and testimonials about nutrition, training and various health approaches represent individual experiences and what is stated on the site does not guarantee any results for your specific situation. Any choice of a specific way of eating or medical treatment according to a given situation should be made under the guidance of professionals qualified to do so.